
Helping Mom work "Smarter, not Harder"
The Dark Side of Block Feeding
Nipple Hygiene
TMJ Support
Weak Suck After Frenotomy
Clinical tips for IBCLCs

September 25, 2013
Supportive Techniques for Biomechanical Challenges
When a baby's tongue and jaw do not align properly, sucking is less efficient and more effort. In addition to allowing the baby to find a comfortable position at breast and referring for body work to restore muscle balance, fingertip support or traction may be helpful. You may need to experiment with several types of support to see which works best for the individual dyad.
When lip seal is poor on one side of the face, drawing the cheek (a cm or so past the corner of the lips) toward the breast with a fingertip may help the baby transfer more milk.
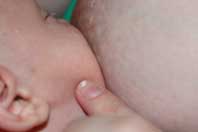
When the jaw is asymmetrical due to torticollis or other restrictive intrauterine positions, the side that is more open may not function as well. Forward traction along the mandible toward the breast may be helpful.
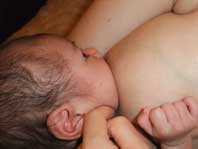
Sublingual support (see Supporting Sucking Skills in Breastfeeding Infants, 3rd edition, page 342) or TMJ support may also help improve support and alignment of the tongue and jaw and improve sucking.
When you've identified the correct technique, the number of times the baby sucks before resting (sucking burst length) will increase and there will be more swallowing and milk transfer.
March 23, 2013
What is involved in a lactation consultation?
An average outpatient lactation consultation takes 1.5 to 2 hours.
During this time, the IBCLC:
- Takes a history of the mother, focusing on any chronic conditions that might affect breast development, hormonal and nutritional support for milk production, and early management of breastfeeding that might affect calibration of milk production.
- Takes a history of the baby, with particular focus on birth interventions and medications, medical procedures required after birth, and feeding history prior to the consultation.
- Assesses the mother's anatomy, neurobehavioral organization and ability to support the baby both physically and emotionally. Assess mother for postpartum mood disorders and psychosocial needs. Assess emotional adjustment to and acquisition of the maternal role. Counsel parents around any issues, provide referrals if needed.
- Assess the baby's neurological functioning (including muscle tone, state stability, autonomic stability), global, craniofacial and oral anatomy and function, bilateral symmetry, any malformations or deformations, and their likely effect on feeding.
- Assess the baby's health and nutritional status, maturity, and feeding skills.
- Assess breastfeeding skills and interactions in both the mother and baby and the dyad as a unit.
- Watch a feeding, looking particularly at postural control, state stability, ability to find and attach to the breast (using sense of smell, hands, cheeks, lips, tongue), the component movements of sucking, suck:swallow:breathe coordination, effort of respiration, ease of initiation of sucking, ability to sustain sucking. Sucking burst organization, milk transfer, ability to feed until nutritional needs are met.
- Assess and evaluate problems identified, rate the relative contribution of each to the breastfeeding difficulties, identify management changes, compensations and facilitations that might be appropriate for the dyad. Confirm observations with oral examination, digital suck exam, breast palpation, cervical auscultation, test weights, etc as needed.
- Apply treatment probes - assess the effect and if successful, teach the new technique to the mother and asses her acceptance/ability to execute it. Allow time for the dyad to practice the new techniques. Educate the mother/parents about WHY you have recommended these things.
- If milk expression is required as part of the plan, teach the mother to express by hand or with her existing breast pump, problem solve expressing problems, problem solve milk production problems. Recommend specific rental equipment if needed.
- Prepare a written care plan, and go over it with the parents.
- Teach parents how to use, care for, and clean any feeding equipment used in the care plan.
- Provide anticipatory guidance, what to expect, signs that feeding is improving, danger signs that mean the health care provider should be seen, when to follow up with the IBCLC.
- Refer the mother to mother to mother support groups (La Leche League, Breastfeeding USA, Nursing Mother's Counsel, Baby Cafe).
- Write a report to/communicate with the baby's (and mother's, if applicable) primary health care provider detailing findings and interventions and identifying any areas that require medical follow-up.
- Then there's phone and email follow up after the consultation!
January 16, 2013
Helping Mom work "Smarter, not Harder"
Mothers who are experiencing breastfeeding difficulties are often 'triple feeding'- feeding at breast, pumping and then bottle feeding, and then cleaning all that equipment. Often the baby stops working very hard at the breast and spends long periods sucking ineffectively, leaving the mother without time to express milk frequently enough to increase her milk production, and the whole thing becomes unsustainable. An appropriately chosen at-breast supplementer can reduce the time spent feeding and improve breast drainage, stimulating increased milk production.
My usual goal is to keep the feed-express-clean cycle down to less than an hour per feeding. Forty minutes is even better, as this is comparable to the maximum time a healthy newborn feeds. The baby's previous growth and oral motor strength will determine which supplementer will allow sufficient reward for working at the breast and produce milk removal from the breast as well as the device. A baby who is below birth weight at two or three weeks of age needs much more support than one whose growth has been marginal but suboptimal. For infants with very low strength or stamina, use a 5-french feeding tube attached to a syringe of milk and give the baby a small bolus of milk with every suck by pressing on the plunger. Watch the baby - if the flow is too fast, the baby will spill some milk from the lips or show stress cues (splayed fingers, wide open eyes, etc). If the flow is too slow, sucking bursts will be short and the baby will require prodding to start sucking again. Make sure that parents know how to distinguish respiratory pauses from 'giving up', it's important to pause giving flow when babies stop sucking to breathe. (Babies who consistently use short sucking bursts along with rapid, panting or noisy breathing may have cardiac or respiratory malformations. See Supporting Sucking Skills in Breastfeeding Infants, 2nd edition, chapter 8 for more information on safely feeding infants with structural issues.)
If the baby is vigorous but mom has reduced milk production due to primary issues (hypothyroidism or breast surgery) or secondary ones (poor "market research" due to early separation or supplementation), a Lact-Aid Nursing Trainer is an ideal supplementer. This supplementer requires the baby to suck using negative pressure, so it usually allows good milk flow from the breast as well. A tube in a bottle Lactation Aid ala Dr. Jack Newman (see previous article on Weak Suck After Frenotomy) can also be used for vigorous babies, with mother holding the bottle at nipple height or lower to encourage normal sucking pressures. The Medela Supplemental Nursing System can be used as well. For vigorous infants, the yellow cap should be at nipple height and the medium tubing used. If the baby cannot get a full meal from the breast and device in 40 minutes or less, elevating the container or using larger tubing, or venting one tube can all be tried.
Dyads that fall between the extremes provide more of a challenge in choosing tools. In this case, I often start with the syringe and tube or tube in a bottle with the bottle held above breast height, and as the baby gains strength and stamina, we move onto a commercial device if a longer period of supplementation is needed to help stimulate or re-build mom's milk production. This way mom avoids purchasing an expensive tool until we are more certain the baby can make it work.
Once feeding times are under control, mom will have more time to express milk. Manual expression often works best when milk production is low, and leaves little to be washed afterward! If baby is healthy and full term, mom can use the pump several times in a 4-6 hour period and then clean the collection kit. Making expressing more convenient - supplies in the room mom spends most of her time, perhaps investing in multiple kits so cleaning is not done as often, or refrigerating the kit in a large plastic bag between uses all help. Initially as the dyad is learning to use a supplementer, mom may be able to pump only a few times a day after nursing. Teaching manual expression can make it less of a 'big deal' to express, or waiting until the baby is feeding well with the supplementer to focus on increased pumping can make the plan 'doable'.
For more information about using specific supplementer devices, see Selecting and Using Breastfeeding Tools - soon coming in e-book format!
September 26, 2012:
The Dark Side of Block Feeding
Block feeding is an effective method of reducing milk production in mothers with hyperlactation. If the intervals of time between alternating breasts (blocks) are increased gradually and mothers are instructed to express minimal amounts of milk by hand to maintain comfort, the risk of engorgement and milk stasis, plugged ducts and mastitis are low. Block feeding is problematic when applied to mothers who do not have hyperlactation. Many mothers know about block feeding, and resort to unilateral feeds when their infants are fussy or have difficulty handling milk flow. Sometimes breastfeeding helpers recommend block feeding in a telephone contact when mothers report infant fussiness, without a good feeding assessment and weight history. Block feeding should only be recommended when the infant is consistently gaining more than 8 oz (225 g) per week and has no risk factors for inefficient feeding if the milk production is reduced. Tongue-tied infants may have difficulty handling a normal milk flow, then fail to thrive if mother deliberately reduces milk production. Before advising block feeding, infants should be assessed for dysphagia, tongue-tie, micrognathia, respiratory tract instability (laryngomalacia/tracheomalacia). Test weights are also helpful in determining whether mother's milk flow is excessive due to increased milk production or whether the infant is having difficulty with a normal flow.
August 11, 2012
Nipple Hygiene (Yes, Soap and Water) to reduce infection risk:
Injured nipples provide a highway for bacteria to enter the breast. During the normal mechanics of breastfeeding, milk travels up from the large ducts near the nipple as the milk ejection recedes, drawing saliva from the baby and organisms from the nipple skin as well. This process allows the alveoli to monitor how much milk was taken and the mother's immune system to monitor her and the baby's microbial environment and respond with antibodies. It also opens the mother to breast infection if her nipple becomes colonized or infected. Bacteria produce biofilms composed of proteins and complex sugars (polysaccharides) that help shield them from the immune system and water washing. Soap and mechanical disruption are required to eliminate biofilms.
Sore, reddened nipples have cultured Staph species in several studies.
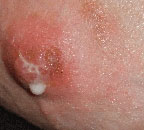
impetigo (staph infection)
Washing with mild soap and water 2-3 times a day was enough to cure 33% of these staph infections in Stephen Grave's et al study of breastfeeding women with nipple pain and redness. Verity Livingston also identified soap and water washing as important to removing staph organisms from infected nipples, along with systemic antibiotics to prevent mastitis, especially when the nipples have a purulent discharge.
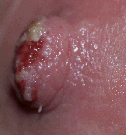
purulent nipple (bacterial infection)
It's wise to counsel mothers having breastfeeding problems to wash their nipples with mild soap and water 2-3 times a day, especially if the nipples are injured. Once breastfeeding is comfortable, using soap in the shower once a day is helpful. Since I've been giving this advice to mothers as soon as they call for an appointment, I'm seeing fewer of them proceed to mastitis and abscess.
July 17, 2012
Supporting the "Popping" TMJ (Temporomandibular Joint)
Body structures need to line up properly in order to work well. Intrauterine positioning can cause deformation of the jaw so the condyle of the mandible no longer fits nicely into the little hollow in the temporal bone of the skull, limiting mouth opening. During the birth process, ligaments or muscles on one side of the jaw can be stretched, displacing the condyle from the little disk that normally cushions the joint. If the condyle no longer tracks with its' disc, the jaw will be unstable on that side. If you place your fingertips gently over the TMJ while the baby sucks, you will feel a popping sensation as the baby opens the mouth when the disc clicks back into place. It is also possible for the disk to be displaced and not return to it's normal position.
Babies having TMJ problems may have difficulty opening the mouth widely enough to latch on deeply, or they may have difficulty getting into a smooth sucking rhythm. Both can cause low milk transfer.
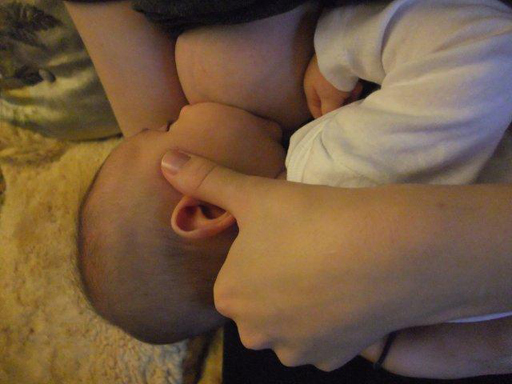
If you suspect that the TMJ is making the baby's sucking efforts less successful, you can try some fingertip pressure above and behind the joint on the affected side (see photo). If this is the right intervention, the joint will feel more stable and the baby will immediately suck more effectively. In this case, you can teach the mother to support the same area while she nurses, particularly when that side of the jaw is facing upward. Mother's arm may provide sufficient support for the jaw when the affected side is facing downward.
Remember that jaw support doesn't eliminate the problem, but may help the baby compensate. Body work (osteopathic or chiropractic treatments, physical or massage therapy, etc) can help restore normal biomechanics. The muscle activity of breastfeeding can also help normalize the bony parts of the face over time.
July 11, 2012
Helping babies improve negative pressure sucking after frenotomy:
While many infants suck properly within days of a frenotomy, some continue to suck weakly, with poor suction (negative) pressures. One method to help gradually increase sucking pressures is to slowly increase the amount of vacuum the baby needs to exert to get milk. One way to do this is to use a lactation aid consisting of a 36 inch 5-french feeding tube placed in a bottle of milk.
At first, hold the bottle high well above the breast so milk will flow down the tubing easily. Find a position for the bottle where the baby uses a 1:1 or 2:1 suck:swallow ratio with a soft, unstressed swallow. Then move the bottle down an inch or two, so the baby needs to work a little harder to generate the same flow. Assess to ensure that the baby is getting sufficient milk (less than 3:1 suck:swallow ratio during active sucking).
Show the baby's mother how to identify active feeding. Advise her to lower the bottle another inch or two every day or so, as the baby tolerates. If the baby gets fussy or fails to have a good feeding, she will need to raise the bottle higher. She may find that the baby needs less assistance at some feedings (typically first thing in the morning when the breasts are more full, and when well rested after a nap) and more help at others. This is fine. We expect that over the course of several days or weeks, the baby will be able to exert sufficient vacuum to breastfeed without the lactation aid. If little to no progress is made, assess the baby again to ensure that there are no other anatomical or medical challenges.
More information on different lactation aids/nursing supplementers and nuances of their use can be found in Selecting and Using Breastfeeding Tools.

If you purchase through this link, I get a small commission. Thank you!
Feedback

Share your own nuances. Email your submissions to: vincent.genna@gmail.com. Please include "comment" and the title of the post in your subject line, and your name and credentials if you would like them posted.
Home








